Medical Negligence and Injuries to the Bile Duct


A study by the University of Oxford found that bile duct injury accounts for the largest proportion of negligence claims following laparoscopic cholecystectomy in the UK.
In the UK, claims for compensation in respect of bile duct injuries and hospital negligence frequently succeed (most commonly, by way of settlement out of court). This study contained data from a 15 year period to 2009 and in this period, 65% of the cases studied were found in favour of the patient. This study also reported that the average cost of compensation per patient was above £50,000. In the USA, the findings are similar but the compensation amounts are much higher.
This study showed that opinions differed in relation to who was at fault in cases of bile duct injury. Poor decision making by medical professionals was the most commonly identified reason for bile duct injuries but almost half of research respondents identified factors outside the surgeon’s control as being the most important cause of bile duct injury.
Medical Negligence Solicitor
Helen Coughlan is a partner and advises on medical negligence*, family law and personal injuries*. Helen is a qualified family mediator and collaborative law practitioner and is Chairperson of the Family and Child Law Committee of the Law Society.
Medical Negligence Solicitor
Emma Farrell is a partner and advises on medical negligence* and personal injuries*. She qualified with the largest solicitors’ firm in Ireland and has significant expertise.
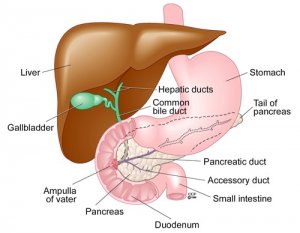
The Cleveland Clinic explains that the gallbladder is a small, sac-like organ that sits under the liver on the right side of your abdomen (belly). The gallbladder stores a greenish fluid called bile. Bile is made and released by the liver and then sent to the small intestine, where it helps the body break down and absorb food. Bile moves through a network of tube-like structures called bile ducts.
Gallstones are small stones that form in the gallbladder. Usually, they consist of cholesterol. According to HSE data, if you have gallstones, in the majority of cases, you won’t need treatment and you won’t have any symptoms.
The risk of gallstones is higher if you are:
When you have symptoms caused by gallstones, this is called gallstone disease or cholelithiasis. The HSE advises that treatment is necessary if gallstones are causing:
A HIQA report explains that the symptoms arising from sudden and complete obstruction of the cystic duct or the common bile duct by a stone is called ‘biliary colic’.
In some cases, you may need surgery to remove the gallbladder. This is often known as a laparoscopic cholecystectomy and the HSE note that there is generally a low risk of complications. The Cleveland Clinic explains that the benefits of laparoscopic cholecystectomy (ie, keyhole surgery) over open surgery include less pain, less time in the hospital and quicker recovery. They state it is now considered the “gold standard” for surgical treatment of gallbladder disease.
The same report by HIQA noted that biliary calculi (that is, gallstones) are one of the most common surgical problems in the western world. Gallstone disease is the most common abdominal condition for which patients are admitted to hospital in developed countries.
Further, it states that gallstones are at least twice as common in women and that the increased risk in females begins at puberty and is increased further with the use of the oral contraceptive pill; while indicating that patients with a body mass index (BMI) greater than 40 Kg/m2 have shown a risk of developing gallstones that is eight times higher than those with a lower BMI.
If you would like to read further information on gallstones, click here.
“I would give the service an a ten absolutely. I was provided with the pros and cons regarding how a case like mine could go from the start. This gave me sufficient information to make my decision as to whether to proceed or not. I appreciated having the facts from the outset. From reception to the solicitors I dealt with, everyone was friendly and efficient. I will definitely recommend you to others.”
If you would like to speak to a solicitor about medical negligence involving damage to the bile duct, please call 045 431542 and ask to speak to Helen Coughlan or Niall Farrell who are medical negligence solicitors with experience in bile duct cases.
The NHS in the UK reports that surgery to remove the gallbladder (also known as a cholecystectomy) is relatively safe procedure, but like all operations there’s a small risk of complications. Some of the possible complications are the following:
During the operation to remove your gallbladder, your bile duct can be damaged. Sometimes, the damage can be repaired straight away but in other cases, the damage can be more long lasting.
Similarly, your surrounding organs can be damaged as part of the surgery.
After the gallbladder is removed, sometimes bile fluid can leak into the abdomen. Sometimes a further operation is required to drain this bile.
A HIQA report notes that the most serious complication of cholecystectomy (open and laparoscopic) is damage to the common bile duct. It states that the incidence of bile duct injuries varies between 0.1% and 0.3%. The report notes that other complications of cholecystectomy include bile leak, peritonitis requiring re-operation, postoperative bleeding requiring operation, and intraabdominal abscesses requiring operation. The laparoscopic approach is associated with a lower rate of surgical site infection when compared with the open procedure.
The NHS advises that it will usually take two weeks for you to return to your normal activities if you have a keyhole (or laparoscopic) surgery. If you have an open procedure, it will take longer (around 6 to 8 weeks). There can be temporary side effects from the surgery feeling sick or painful wounds. However, the NHS advises you to contact your doctor if you experience the following as they could be a sign of a complication of the surgery:
If you would like further information, click here.
The Cleveland Clinic explains that during surgery, a bile duct can get cut, burned, or pinched. As a result of an injury, the bile duct will not be able to work right, leaking bile into the abdomen or blocking the normal flow of bile from the liver. Bile duct injuries lead to symptoms that can be painful and dangerous if not treated.
Some studies estimate that bile duct injuries occur in 1 in 1,000 cases of laparoscopic gallbladder surgery. They appear to occur less often in open surgeries. The Cleveland Clinic notes that most bile duct injuries that occur during gallbladder surgery happen because the area around the gallbladder and bile ducts is masked in some way so that the doctor cannot see it clearly. This can happen if the area’s structure (anatomy) is different than normal, or if there is a lot of bleeding, swelling, or scarring in the area.
They say that some doctors think that using a test called intraoperative cholangiography (IOC) more often will help reduce the number, or severity, of bile duct injuries, while other doctors believe that not all injuries can be prevented, even with IOC. Other doctors suggest that changes in how the surgery is performed and the equipment used will reduce the number of injuries. However, not all bile duct injuries can be prevented, so they remain a possible risk of gallbladder surgery.
The University of Oxford study reported that factors that may contribute to bile duct injury include anatomic variation, severe inflammation, errors related to skill, knowledge or judgement of the medical professionals or demographic factors such as patient age or sex.
The Cleveland Clinic notes that the patient outcome depends on the type and extent of the injury and how soon the injury is found. Most bile duct injuries can be successfully repaired, and the patient can go on to have a good quality of life. In severe cases, with more than one surgery, many months of recovery might be needed.
If you or a loved one has suffered from a bile duct injury as a result of medical negligence, you can take the following steps to pursue a claim:
The first step in seeking compensation for a bile duct injury is to consult with a solicitor experienced in medical negligence and delayed diagnosis claims. They will guide you through the process and assess the merits of your case. An experienced solicitor will be able to determine your eligibility and advise you on the likelihood of your claim’s success.
Patrick J Farrell Solicitors specialise in the area of medical negligence, if you have been affected by a delayed diagnosis, don’t hesitate to contact us regarding your concerns and to receive expert advice. If you have suffered a bile duct injury, we can advise you on whether or not you may have a case.
We have acted in successful cases where our clients have suffered common bile duct injuries as part of laparoscopic cholecystectomies for gallstones. The majority of these cases resulted in our client having to undergo further surgery to address the issue. Our medical experts identified flaws in the surgery and aftercare and were often critical of the record keeping of the hospitals. Lack of adequate record keeping is often a very frustrating element of the process for our clients as they try to establish what went wrong with their surgery.
Your solicitor will request your complete medical records, which are crucial for supporting your claim of a delayed diagnosis. This includes your full medical records, any correspondence with the medical practice or practitioner, and other documentation related to your care. These pieces of evidence are essential for establishing that negligence occurred.
To support you in your claim, we can take up your medical records and obtain a medical report which will assess your injuries and examine whether anyone was at fault. At that stage you can decide whether or not it is appropriate to proceed with a claim. We have access to specialist medical consultants, generally in the UK, who will prepare these reports.
If necessary, you may need to have an independent medical expert evaluate your case and whether the care you received constituted negligence.
Once your solicitor has gathered all necessary evidence, they will draft a Letter of Claim and notify the medical practice/practitioner that you intend to take a case against them. Your Letter of Claim outlines the details of your claim, the alleged cause of negligence leading to a delayed diagnosis, and the subsequent consequences for your health.
The doctor or medical practice, through their own legal team, will respond to the Letter of Claim. They may accept responsibility and offer a settlement for any harm or suffering; or they may dispute the claim which will lead to further legal proceedings. Many claims are settled out of court. Your solicitor will negotiate on your behalf in order to receive fair compensation for your injuries, any costs incurred, and any future care needs.
However, if a settlement can’t be reached, your case could proceed to court where your solicitor will represent you in any court proceedings.
At Patrick J. Farrell & Company Solicitors, we understand that undergoing surgery or medical treatment involves a tremendous amount of trust in healthcare professionals. When that trust is broken through negligence—particularly in complex procedures like gallbladder surgery or endoscopies—the consequences can be life-altering.
We Focus on Medical Negligence Claims Involving Bile Duct Injuries and Surgical Errors
Among the most serious—and often preventable—surgical complications are bile duct injuries and accidental nicking of the intestines. These errors frequently occur during procedures such as laparoscopic cholecystectomy (gallbladder removal), ERCP, or abdominal surgeries. They can lead to:
If this has happened to you or a loved one, you are not alone—and you have legal rights.
Case Highlight: Brendan Ward v South Western Health Board & Others
One of the most striking examples of surgical negligence in Ireland was the case of Brendan Ward, a 39-year-old man who underwent an ERCP procedure in 1998. What should have been a routine investigation turned into a nightmare when he developed severe acute pancreatitis due to medical mismanagement. He suffered life-changing neurological damage and had to undergo extensive surgery and rehabilitation.
After a prolonged legal battle, the defendants admitted negligence, and Mr. Ward was awarded €247,000 in damages. The High Court recognised not only the avoidable nature of the procedure but the lack of proper informed consent and post-operative care.
You Deserve the Same Standard of Justice
At Patrick J. Farrell & Company, we’ve built a strong reputation for representing individuals harmed by negligent medical care. Our experienced team of solicitors works with medical experts and independent specialists to thoroughly investigate your case, ensure accountability, and pursue the compensation you deserve.
We handle claims involving:
Bile Duct Injuries can have a significant impact on health and well-being of patients, and may lead to months of recovery.
If you or a loved one has suffered due to an bile duct injury caused by negligence, it’s important to seek expert legal advice to obtain a thorough understanding of the complex legal and medical issues involved – and, most importantly, to ensure you receive the justice, closure and compensation you are entitled to.
If you would like to speak to a solicitor about medical negligence involving damage to the bile duct, please call 045 431542 and ask to speak to Helen Coughlan or Niall Farrell who are medical negligence solicitors with experience in bile duct cases.
At Patrick J Farrell & Company Solicitors, we understand the profound impact medical negligence can have on your life. With a legacy founded by Patrick J. Farrell and carried forward by a dedicated team, we have been advocates for justice for over four decades. Our commitment to putting our clients’ interests first, combined with our extensive legal expertise, makes us the ideal partners in your pursuit of justice.
From the moment you walk through our doors to the resolution of your case, you’ll be treated with the utmost courtesy, respect, and understanding. Choose us – where your well-being is our top priority. Reach out to us today and let our experienced solicitors guide you every step of the way.
Delayed Diagnosis ClaimsHow To Make a Medical Negligence Claim
Making a Medical Negligence Claim
Birth Injury Claims: Guide to Concerns and Compensation
Will Irish healthcare issues cause an increase in medical negligence claims?
Plastic Surgery and Cosmetic Procedures
Hip replacements and joint replacements
Understanding Healthcare-Associated Infection (HAI) Claims
Hip replacements and joint replacements